 Service Overview — Non-Standard Contract Types
Service Overview — Non-Standard Contract Types
Many long-time athenahealth clients have service contracts that pre-date our current, more comprehensive service offerings, namely, athenaOne and athenaOne for Hospitals & Health Systems.
athenahealth continues to support our service agreements for clients who have these older, "non-standard" contract types:
- athenaCollector (No Posting)
- athenaCollector (No Followup)
- athenaClinicals (No Collector)
Tip: You can see your athenaCollector service level at the very top of your screen, on the leftmost tab of the Web browser. You can also pause your cursor over the tab to view your practice name and practice ID number. 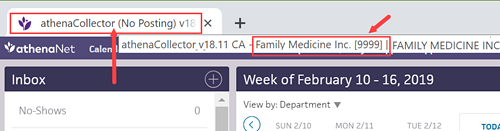
Your organization is responsible for follow-up of all claims in BILLED, HOLD, MGRHOLD, CBOHOLD, MISSING, FOLLOWUP, APPEALED and OVERPAID status; and for posting remittance information. athenahealth is responsible for claims in DROP and ATHENAHOLD status.
Because all correspondence is mailed to directly to your organization, athenahealth does not complete posting work.
If athenahealth receives mail intended for your organization, athenahealth sends it to the address recorded under Set Practice Mail Return Address on the Practice Addresses page: On the Main Menu, click Settings ![]() >Practice Manager. In the left menu,under Practice Links — Miscellaneous, click Practice
Addresses.
>Practice Manager. In the left menu,under Practice Links — Miscellaneous, click Practice
Addresses.
Exception: Live checks are sent through the live check return process before they are mailed to the address noted on the Practice Addresses page.
athenahealth claim actions are limited to research and payer contact to resolve claims landing in an ATHENAHOLD status or held in a DROP status.
There are many kick codes that are available for use by your organization to manage your outstanding claims:
CALLBACK — To be used when your organization has contacted a payer via voicemail, fax, or email and is awaiting a response.
The claims move to a BILLED status.
CHECKSRCH — To be used when needing to pend a claim due to a check being issued by a payer between 30-60 days prior and has still not been cashed. Typically, the payer has advised your organization to allow more time to receive the check, receipt and EOB for posting.
The claim moves to a BILLED status.
NORESPPAYORCALLED — This system kick code will be applied to a claim if no response has been received since the PAYORCALLED kick was applied.
The claim moves to a HOLD status.
PAYORCALLED — To be used when your organization has made a telephone call to a payer and a message was left requesting a call back.
The claim moves to a BILLED status.
PRACTICERVW — To be used when a user in your organization would like a claim reviewed by a practice manager in your organization.
The claim moves internally to a FOLLOWUP status.
SENTAPPEAL — To be used when your organization needs to indicate that a claim was not paid but there is cause to appeal. The appeal process has begun.
The claim moves to a BILLED status.
SHAREDTINREMITREQ — To be used when your organization requesting the EOB/Payment information from another entity with the same TIN.
The claim moves to a BILLED status until the EOB can be uploaded for posting.
SHAREDTINREMITREQ2 — To be used when your organization has escalated the last EOB request after not receiving a response.
The claim moves or stays in a BILLED status until the EOB can be uploaded for posting.
SHAREDTINREMITSENT — To be used when your organization has received all applicable documentation and has since routed it all to athenahealth for posting to be completed.
Your organization is responsible for reviewing and acting on all claims in BILLED, HOLD, MGRHOLD, FOLLOWUP, CBOHOLD, MISSING, APPEALED, and OVERPAID status. You will be able to dispute timely filing denials by contacting athenahealth to request proof of timely submission; this is valid for electronic claims. athenahealth is responsible for the claims in DROP and ATHENAHOLD status, and for posting remittance information.
athenahealth will post remittances received from insurance payers; we will also perform posting or unpostable related follow-up. Items received that do not have a match in athenaOne will be assigned to your organization in the Remittance Dashboard, if athenahealth is not able to resolve.
athenahealth will not perform any follow-up or denials management actions on your claims. It is your organization's responsibility to review, research and resolve all claims billed through athenaOne; this includes appealing and resubmitting corrected claims.
Claim alarms will fire to indicate that a payer has not provided remittance; when this alarm fires claims will be routed to the FOLLOWUP work queue for your organization to perform next actions.
When remittance is received indicating a payer denial, the claims will be routed to CBOHOLD for the denial or error to be corrected by your organization. Your organization can use a set of kick codes to address outstanding claim issues.
There is no billing, posting, or claim follow‑up included with this service.