CMS Reporting Dashboard
athenahealth Population Health
Use this page to report and review data for CMS ACO quality measures relevant to your organization. For more information, see these documents: GPRO Guide to Success and Group Practice Reporting Option (GPRO) Workflow Template.
On the Main Menu, click Quality. Click Network CMS—ACO Dashboard
Your organization must use athenahealth Population Health, and you must have a role that includes the Population Management: CMS ACO Population permission to use the CMS Reporting Dashboard.
To view the Quality Manager page, you must have the Population Management: Quality Manager permission. In addition, you need the Population Management: Quality Manager: Exclusions permission to exclude patients from quality measures.
To view the Quality CMS ACO Scorecard - PCP report, which tracks quality compliance for a CMS ACO reporting period, you must have the Population Management: Quality CMS ACO Scorecard - PCP permission. (This permission is in the Quality section of the report permissions list.)
In 2010, the Centers for Medicare and Medicaid Services (CMS) created the Group Practice Reporting Option (GPRO) requirement for Accountable Care Organizations (ACOs). CMS GPRO web interface quality reporting occurs during the first quarter of each year for the previous measure year for all CMS ACOs (including MSSP tracks and Next Generation ACO).
CMS measures the quality performance of an ACO. athenahealth Population Health provides the data aggregation, manual workflows, service experience, and GPRO-specific support to help your organization during the reporting process for the Web interface quality measures.
Note: The primary care physician in the ranking file is not the same as the primary care physician in the athenahealth Population Health tool, which is based on your provider attribution logic. If you have questions about your attribution logic, please consult your Customer Success Manager.
To satisfy GPRO web interface quality reporting, your organization must report on a minimum of 248 patients in consecutive order (or all patients in the sample if there are fewer than 248). The general reporting steps include:
- Confirming that the sample patient is eligible for the measure (population confirmation, exclusions).
- Documenting that the relevant results exist in your EMR (numerator compliance, exceptions).
The Population Health CMS Reporting Dashboard is a tool to help you accelerate the process of GPRO tracking and reporting on the quality measures for the CMS program. Through the Quality Manager, you can track and close quality gaps for your patients throughout the year.
You can access and download the patient ranking file and discharge XML file for the performance year from the CMS GPRO Web interface.
- Patient ranking file — a list of beneficiaries (up to 616 per measure) sampled for reporting — includes the quality measures that the beneficiary was sampled for, the rank of the beneficiary within the sample, demographic information, and the beneficiary's primary care physician.
- Discharge XML file contains the discharges that should be reported on for the medication reconciliation measure.
Note: The only way to access your patient ranking file for a performance year is from the GPRO Web interface. The file is not provided via Managed File Transfer (MFT). If your ACO does not have the necessary EIDM account and roles established, you cannot access and download your patient ranking file. If you need assistance, please contact your Customer Success Manager.
To use the CMS Reporting Dashboard, upload your patient ranking and discharge files to the athenahealth GPRO folder via SFTP. Then, within 1 week, athenahealth uploads the files into the CMS Reporting Dashboard.
During the GPRO reporting period, you must complete reporting for 248 consecutively ranked patients in ranked order. For example, you must successfully report on a patient ranked #1 for a measure to receive credit for reporting on any other patients in the ranked list.
athenahealth produces the XML file and posts it on SFTP once during the reporting period for you to upload into the CMS GPRO tool. The XML file produced by athenahealth is based on the specifications that CMS posts each November.
The CMS Reporting Dashboard displays an overall status for each test within the CMS program.
Note: Overall progress (total reporting progress) is the default view for this page.
The tests are organized by module (such as Care Coordination), and each test contains the following information in these columns.
Note: If your organization includes more than one ACO, these columns are calculated by measure for each ACO: Completed with data, Completed without data, Incomplete with data, and Incomplete without data.
Quality test
The name of the test. To display a short description of each measure, hover the cursor over the Information icon ![]() next to each test.
next to each test.
Overall progress
The percentage of beneficiaries by measure that you have completed reporting for (not necessarily in ranked order). To display the percentage of beneficiaries who could be reported as complete in consecutive ranked order by CMS reporting standards, you can switch the view from Overall progress to Reporting status. You can see completeness gaps on the tracking bar.
Next incomplete patient
The next ranked beneficiary for whom the reporting status is incomplete.
Completed with data
The number of beneficiaries who are completed by CMS reporting standards, including population confirmation. Population confirmation is the affirmation that the beneficiary is eligible for the measure and should be in the denominator. If a patient has an exception for a test but has a population eligibility confirmation, the patient is included in the Completed with data column.
Completed without data
The number of completed beneficiaries who do not have a result logged for the test in question, but for whom a population confirmation has been logged (these beneficiaries are considered complete by CMS reporting standards, but not satisfied for the measure).
Incomplete with data
Patients who do not have a population confirmation for a test are considered "incomplete." This column displays the number of beneficiaries who are completed by CMS reporting standards but have not received population confirmation showing that the patient is eligible for the measure. For example, a beneficiary sampled for the colorectal cancer screening measure who had a colonoscopy within the measure year, but was not confirmed as part of the population, is included in the Incomplete with data column. Also, a patient who has an exception for a test but does not have a population eligibility confirmation is included in this column.
Incomplete without data
Patients who do not have a population confirmation for a test are considered "incomplete." This column displays the number of beneficiaries who are incomplete by CMS reporting standards and who do not have population confirmation completed. For example, a beneficiary sampled for the colorectal cancer screening measure who did not have a colonoscopy within the measure year, and was not confirmed as part of the population, is included in the Incomplete without data column.
Excluded
The number of beneficiaries who are excluded from the CMS quality measure. Sample exclusions and medical exclusions are included in this group. Exclusion reasons vary for each measure. For more information, see "To document an exclusion to a CMS quality measure."
Note: The Excluded column may not be accurate until the CMS patient ranking files are loaded.
Total patients
The total number of beneficiaries ranked in the quality test, which for most tests is 616 patients per measure. This total is the sum of these columns: Completed with data, Completed without data, Incomplete with data, Incomplete without data, and Excluded.
Note: CMS may not be able to provide the complete sample of 616 beneficiaries in the case of ACO31 because it may be difficult to determine from the claims data available to CMS whether a beneficiary has LVSD (LVEF < 40% or Documented as Moderate or Severe). Therefore, CMS may rank fewer than 616 beneficiaries for ACO31 and potentially fewer than 248. If fewer than 248 beneficiaries are ranked, reporting should be completed for all beneficiaries ranked.
You can use a Perspective filter when you open a patient list from the CMS Reporting Dashboard. Select an option from the Perspective filter on the filter bar or by clicking Show Filters.
The default filter is Plan Only. Plans may send you a roster of members. Therefore, you see only ranked patients for each CMS ACO measure. To view all Medicare patients — ranked and unranked — who are currently at risk for a measure, select the Current Members filter.
Note: CMS must assign a rank to each patient. If you have no patients assigned a rank for the selected measure year, no patients appear in the CMS Reporting Dashboard.
Additional features allow you to:
- Filter the patient list by PCP, payer, or Medicare data provider (click Filter or Show Filters).
- Review the numerical value of test results in this dashboard, without opening a patient's Person Center.
- View patients excluded from a CMS ACO measure.
- Export a patient list to Excel.
From the CMS Reporting Dashboard, you can click a beneficiary name to open a window which shows patient events, activities, and providers related to the status of the quality measures for that patient. This information also appears in the Person Center Quality tab for that patient. You can view all tests that include this beneficiary in the denominator and whether the beneficiary was ranked for particular measures.
Note: You can use the Person Center Quality tab throughout the year to verify whether a patient would be satisfied for the measure.
To the left of each measure, red and green bars indicate the patient's compliance status for that measure (green = compliant; red = not compliant). To the right of each measure, the reporting status indicates whether the patient has satisfied the measure for GPRO purposes.
- The green and red indicators on the left consider all data sources, including payer claims.
- The reporting status on the left considers only EMR and manual data sources for GPRO reporting.
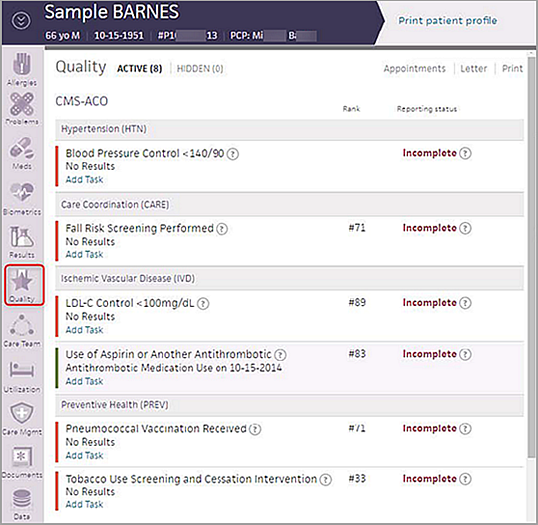
In this example, the patient is compliant for the Use of Aspirin measure (green bar to the left), but the reporting status is still Incomplete because you need to confirm the patient's eligibility for the measure to finish the reporting during the GPRO period.
Note: For information about the reporting status, hover the cursor over the tooltip icon ![]() to the right of the reporting status (Complete, Incomplete, or Excluded).
to the right of the reporting status (Complete, Incomplete, or Excluded).
To begin documentation for a particular quality test:
- Display the CMS Reporting Dashboard: On the Main Menu, click Quality. Click Network CMS—ACO Dashboard.
Each test within the CMS program is displayed by module (for example, Care Coordination and Preventive Health) with the overall reporting status for each test.
Note: For a description of each column on the dashboard, see "Columns on the CMS Reporting Dashboard." - Click the row of the appropriate test.
You see a list of beneficiaries who are complete or incomplete for that test. You can sort and filter this list.
Note: The dashboard provides additional descriptions related to the reason that the beneficiary is associated with a "Completed" or "Incomplete" test reporting status. The "No Results (see related claim)" description is helpful when trying to locate the clinical data in the EMR (you can identify the related claim and note the data associated with the claim). - From the Reporting Status filter, select Incomplete to display a full list of patients for whom reporting must still occur.
- Click a beneficiary name in the patient list to display more quality test information for that patient. You can view all tests that include this beneficiary in the denominator and whether the beneficiary was ranked for particular measures.
- Click a test to expand the row and enable data entry for that test. Complete the test dates, as well as results and exclusions (if applicable).
Note: For individual test workflows, see the Group Practice Reporting Option (GPRO) Workflow Template. - Perform a population confirmation by selecting a year in the {Test Name} Population Eligibility Confirmed field. Population confirmation is the affirmation that the beneficiary is eligible for the measure and should be in the denominator. This step is required for all beneficiaries who are not excluded from the test. All patients should have a population confirmation or exclusion documented (do not enter both).
Note: Reasons to exclude a beneficiary from the denominator include: Deceased, HMO Enrollment, In Hospice, Medical Record not Found, Moved out of Country, and Not Qualified for Module/Sample due to not meeting the denominator requirements. - Enter dates and values depending on the measure requirements to satisfy numerator compliance for each measure.
Note: You may need to enter a CMS approved exception if the patient could not meet the numerator — for example, due to Medical Reasons, Patient Refusal, or System Reasons. These exceptions pertain to the numerator for the measure. - To move to the next beneficiary in the patient ranking list for this test, click the Next arrow (to the right of Patient X of Y) at the top right of the page.
On the CMS ACO Dashboard, you can see your progress in two views.
- Overall progress view — Shows you how many patients you have completed entering data for, regardless of rank order.
- Reporting status view — Shows you how many patients you have completed so far that meet CMS reporting requirements.
To view your overall progress, display the CMS Reporting Dashboard Overall progress view. As you complete reporting for more beneficiaries in the ranked list, the percentage increases and the tracking bar fills with the color teal to show real-time measure completion progress.
Note: Overall progress may never reach 100% because 100% means that all 616 beneficiaries were reported on. CMS requires reporting for 248 consecutively ranked patients in ranked order.
For more information, see these documents: GPRO Guide to Success and Group Practice Reporting Option (GPRO) Workflow Template.
On the date agreed upon with your Customer Success Manager, cease reporting in the athenahealth CMS ACO Dashboard, wait for the XML file to be produced by athenahealth, upload the XML file to GPRO, and then continue working in GPRO until the end of the reporting period.
athenahealth provides access to the Quality Manager throughout the upcoming performance year to track and close quality gaps for your patients.
- Display the CMS Reporting Dashboard: On the Main Menu, click Quality. Click Network CMS—ACO Dashboard.
- Scroll down to the measure of interest.
- Click the name of the patient in the Next incomplete patient column.
The Person Center Quality tab for the next incomplete patient in rank order opens. - Click the same test that you selected on the CMS Reporting Dashboard.
The area expands to display the fields used to enter test results.
Note: You can click the Year option to add the reporting year to all measures. The reporting year is displayed in the END DATE field at the top of the page.
Year option to add the reporting year to all measures. The reporting year is displayed in the END DATE field at the top of the page. - Enter the test result information.
- Date — Specify the date that the patient received the test.
- Result — Enter the test result in the second field, if applicable.
Note: This field appears for outcome tests only. - Notes — Enter any notes (optional).
- Click Save.
The application saves the results and marks the patient complete for the selected measure. - Click the Next arrow (to the right of Patient X of Y) at the top right of the page.
The Person Center Quality tab for the next patient opens. - Repeat steps 4 through 6 for the selected patient and test.
- John Smith, a provider at Seven Hills Medical Group, wants to enter the results for all patients who are incomplete for the ACE Inhibitor or ARB Therapy measure.
- He displays the CMS Reporting Dashboard, finds the measure of interest, and clicks the number of patients listed with a reporting status of Incomplete without data.
- The list of these patients is loaded. They are automatically sorted by rank, so John can complete data entry for the patients in rank order for this CMS ACO measure.
- John clicks the first patient in the list and is directed to her Person Center Quality tab. He has that patient's EMR open in another window and, referring to the patient's EMR, enters data for this measure.
- When this patient is complete, John clicks Next. The Person Center Quality tab for the next incomplete patient in rank order appears.
- Display the Quality Manager page: On the Main Menu, click Quality. Click Network Quality Dashboard.
- Click Goal not reached in the CMS-ACO program section of All Quality Programs.
The area expands to show a list of CMS ACO measures. - Scroll down, if necessary, and click the desired test.
A list of patients with no results for the selected test appears. - Enter a date for the desired test to the right of the patient's name.
The application saves the data and updates the number of patients required to reach the selected test's goal.
Note: To enter notes as well as a date for the test results, click the patient's name in the list.
- Display the CMS Reporting Dashboard: On the Main Menu, click Quality. Click Network CMS—ACO Dashboard.
- Next to the measure of interest, click the desired patient group (for example, click the number of patients listed as "Incomplete with data").
- In the Description column of the patient list, you see the entry Current Result (XYZ) for certain patients. This entry refers to a patient's most current test result.
Note: You can click the Description column to create custom worklists by selecting one or more filters. - To see only patients with a result documented, select Current Result from the Description menu.
After the list loads, you can see the numerical value of the result for any outcome measures.
Note: You must have the Population Management: Quality Manager: Exclusions permission to exclude patients from quality measures.
- Display the Quality Manager page: On the Main Menu, click Quality. Click Network Quality Dashboard.
- Click Goal not reached in the CMS-ACO program section of All Quality Programs.
The area expands to show a list of CMS ACO measures. - Scroll down, if necessary, and click the desired test.
A list of patients with no results for the selected test appears. - Click the name of the patient in the patient list. An expanded patient view appears.
- Click
 Document an exclusion.
Document an exclusion.
The Exclusion field appears. - Enter a date in the Exclusion field.
Note: Exclusion dates are keyed to the END DATE that appears at the top of the Quality Manager Details page. To change the end date, click END DATE: YYYY at the top of the page, select a new year from the list of years, then click Apply. - Exclusion reason — Select a reason for the exclusion from the list (the list is organized by Exclusions and Exceptions). Your selection helps you specify whether the patient should be excluded from the measure altogether or whether the patient is an exception from the numerator of a measure.
- Enter notes (optional) in the field below the Exclusion reason list.
- Click Save.
The exclusion appears in the panel's Events tab. The application updates patient status figures above the patient list.
Note: To view test data for the selected patient in the Person Center, click the patient's name at the top of the panel. - Click Close X to close the patient's panel.
- Display the CMS Reporting Dashboard: On the Main Menu, click Quality. Click Network CMS—ACO Dashboard.
- Next to the measure of interest, click the desired patient group (for example, click the number of patients listed as "Incomplete with data").
-
From the Description menu, select Sample Exclusion. This option refers to patients excluded from the CMS ACO measure.
A list of all patients excluded from the measure appears.
Export a patient list to Microsoft Excel for additional analysis or to share the data entry workload.
- Display the CMS Reporting Dashboard: On the Main Menu, click Quality. Click Network CMS—ACO Dashboard.
- Next to the measure of interest, click the desired patient group (for example, click the number of patients listed as "Incomplete with data").
- Click EXPORT Patient PANEL in the upper right corner.
The data is exported to Excel.